The (illustrated) H's & T's: aka reversible causes of cardiac arrest
Cardiac arrest is the medical term for when the heart stops beating. It's one of the most terrifying situations a doctor can face. When blood isn’t pumping, all cells start to die from a combination of hypoxia (lack of oxygen), and build up of the normal toxins no longer being cleared. Your organs fail, and death is the ultimate result.
In advanced life support there is a set of concepts called the H’s & T’s, which summarise the reversible causes of cardiac arrest. These are all potentially 'fixable' problems that doctors can treat to save a life. Every second matters when trying to re-start the heart. Seconds can be the difference between complete recovery and permanent disability e.g. through hypoxic brain damage, or amputation of limbs in sepsis.
I created this article, my Kickstarter, posters, and a video on the subject, because of a horrific night shift where we faced 3 cardiac arrests, two of which happened at the same time. I realised how difficult and important it was to be able to recall them all rapidly when needed in the panic of an arrest situation, especially as most are ideas that are not easily visualised, such as 'Hydrogen ions'.
So what are they?
The H's
Hypoxia
When there isn’t enough oxygen reaching cells, they start to die. The patient may be breathless and cyanotic. Check for an obstructed airway by looking for angioedema (swelling), foreign bodies like vomit, and listening for stridor (a high pitched inspiratory noise caused by narrowing of the upper airway). Hypoxia can be suggested on a pulse oximeter, and diagnosed using an arterial blood gas test
Hypoxia is treated by securing an open airway, providing oxygen, and ventilating the patient if needed. Sometimes drugs like Salbutamol are used to relax the airways, and adrenaline and steroids reduce swelling if the cause is an allergic reaction.
Hypovolemia
Fluid loss reduces blood volume and thus pressure, reducing cardiac output until the heart stops. Consider fluid losses through sweat, vomit, urine, diarrhoea, and bleeding (internally and externally). Consider medicines which may be worsening the situation, e.g. diuretics (which increase fluid losses), and anticoagulation (which prolongs bleeding).
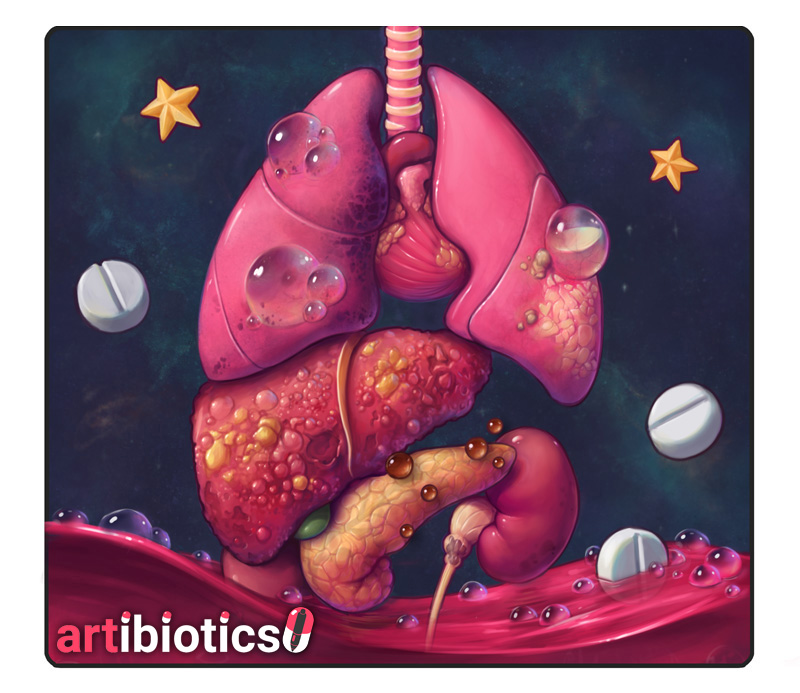
Hydrogen ions (H+)
Raised acidity in the blood prevents normal cell function. It is found via an ABG test, and treated by cause. Consider system failures as causes, including respiratory (e.g. COPD), hepatic (e.g. liver cirrhosis), and renal (e.g. such as obstruction, or an acute kidney injury). Other important causes include sepsis, salicylate overdose, and diabetic ketoacidosis.
Note some stereotypically high potassium foods being lost...
Hypo/Hyperkalemia
Potassium derangement can cause arrhythmias by destabilising the electrical rhythm of the heart. Check the electrolyte levels via an ABG, or venous blood testing. These derangements can also cause changes to the ECG pattern, so it’s worth checking carefully.
Hypothermia
Your body is optimised to work at 37C. Lower body temperatures constrict blood vessels, reduce oxygen availability, and thicken the blood. The heart slows down, and arrhythmia’s lead to cardiac arrest.
It’s a special cause of arrest because resuscitation can be successful long after it’s occurred. The longest documented case was almost 7 hours after a man’s heart stopped when he fell into icy water! It has led to the saying that “you are not dead until you are warm and dead”.
Warming may be used to bring the patient's temperature back into range, e.g. with pre-warmed fluids, or a Bair-hugger device.
The T's
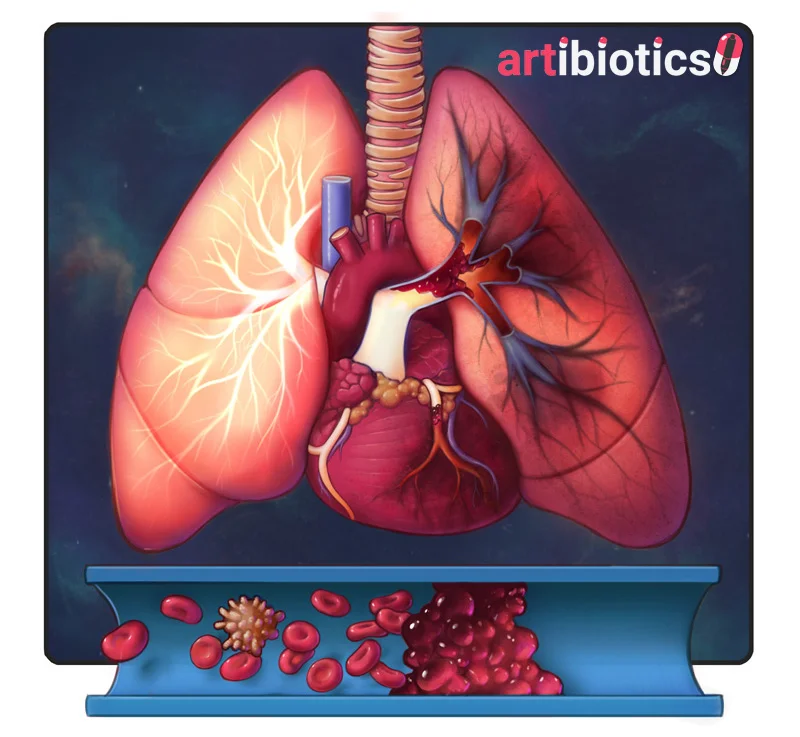
Thrombus
A clot in the hearts supplying vessels causes a myocardial infarction (heart attack). Clots in the lungs are called pulmonary emboli. Blood flow is reduced or stopped beyond this point, resulting in hypoxic death of downstream tissue, and soon the patient if not fixed.
Tamponade
The pericardium is an inflexible fibrous bag that surrounds the heart. If extra material accumulates here, such as blood in a cardiac trauma, it will quickly crush the heart and prevent it from pumping. This can be suggested on a chest x-ray or ECG, but it’s diagnosed with an echocardiogram.
In an emergency, cardiac tamponade can be decompressed with a needle to remove fluid and relieve pressure. The fancy name for this is pericardiocentesis.
Did you notice the bullae on the right lung? These are seen in COPD and are structural weak points, more prone to bursting and leading to a pneumothorax!
Tension pneumothorax
A rupture in the lining of the lung can act as a one-way valve, allowing air to leak into the chest cavity, but not escape. With each breath this mass expands, crushing the heart and lungs until they cannot function, and arrest.
The clinical pattern is breathlessness and hypoxia (through reduced ventilation), and hypotension (through reduced cardiac output). The affected side of the chest will have absent lung sounds, and the trachea may deviate away from the rupture due to mass effect of air outside the lung. It can be seen on chest x-ray.
Tension pneumothorax requires an urgent needle decompression to relieve pressure and restore hemodynamic stability.
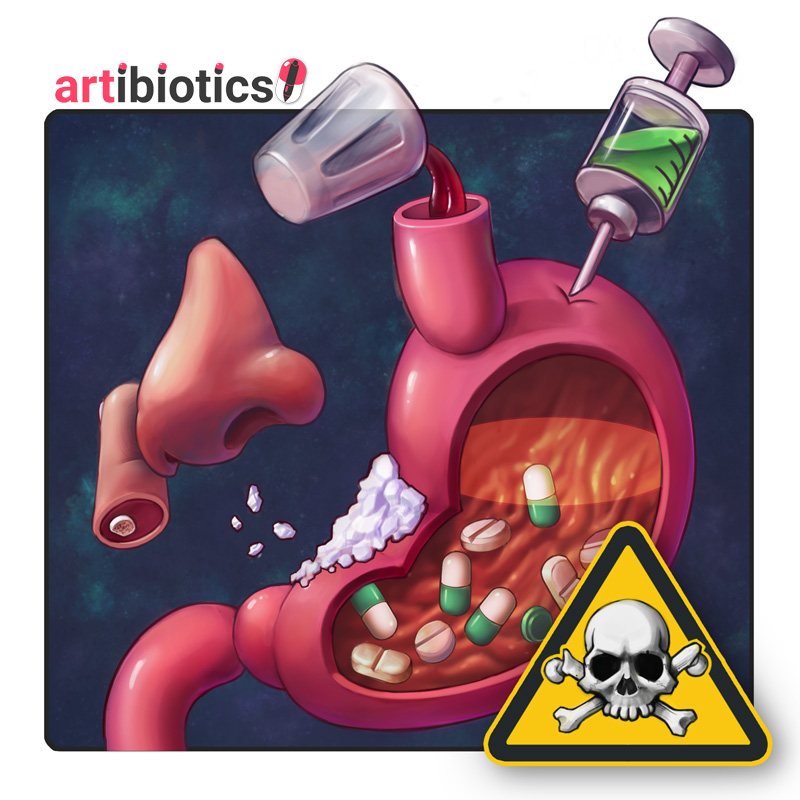
Toxins
Consider overdose of, and anaphylaxis to drugs, including medicines that you may have given. Check the pupils for clues. Stimulants like cocaine will dilate the pupils and can cause vasospasm in the hearts blood vessels, leading to a myocardial infarction. Depressants like heroin and morphine constrict the pupils, and can cause a respiratory arrest.
Conclusion
Note that a proper A to E assessment of the unwell patient is a systematic way to reveal the H’s & T’s, and give you a chance to prevent an arrest from even happening.
That's my quick illustrated rundown on the H's & T's. Anyone who participates in advanced life support should be able to recall them instantly, so they can apply them in the chaos of an arrest situation.
If you’d like to see more from artibiotics then subscribe and follow on the social media we share!